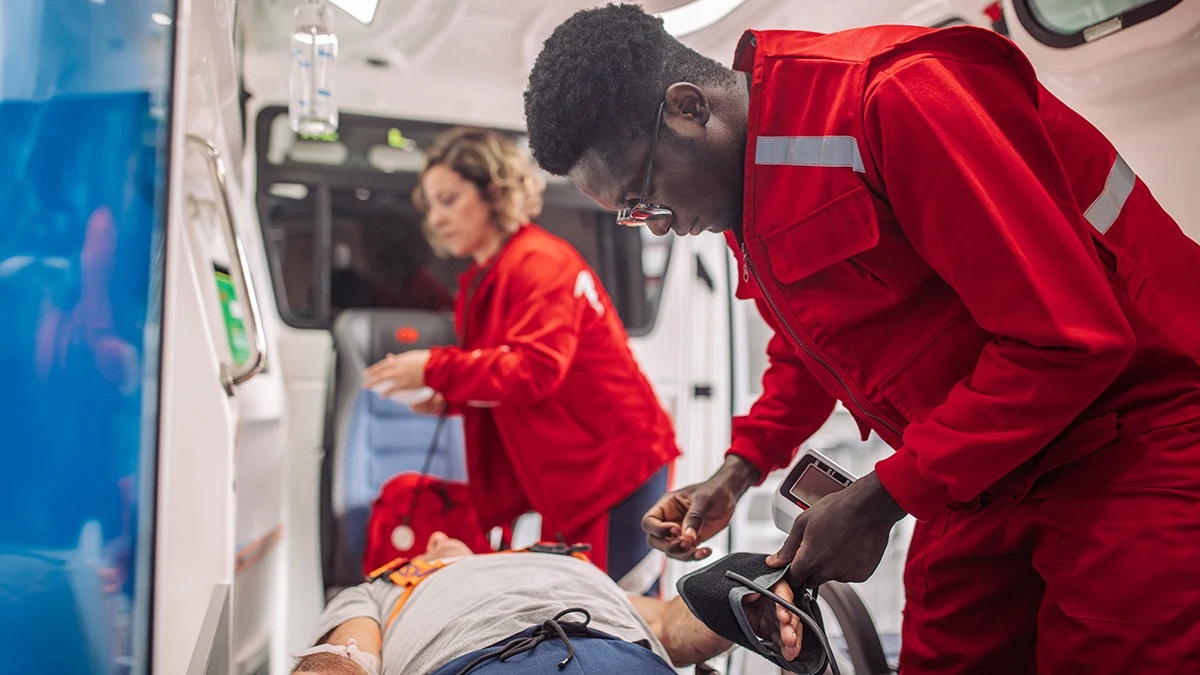
The traditional role of paramedics has been defined by emergency response: arriving at the scene of an acute medical event, stabilizing the patient, and transporting to the nearest emergency department. However, the evolution of community paramedicine and mobile integrated healthcare has expanded the paramedic role into proactive, non-transport care delivery that addresses a significant share of preventable ED utilization. Data on this expanded role demonstrates its effectiveness in reducing unnecessary emergency system activation while improving patient outcomes.
The Scope of Preventable ED Visits
An estimated 13% to 27% (Health Affairs) of all ED visits involve conditions that could be safely managed in lower-acuity settings. Among frequent ED utilizers, defined as patients with four or more ED visits per year, the proportion of potentially preventable visits rises to 40% or higher. These visits are not clinically inappropriate from the patient’s perspective; they reflect genuine healthcare needs that the traditional system fails to meet through non-emergency channels.
The most common conditions driving preventable ED visits include urinary tract infections, upper respiratory infections, minor wound management, symptom exacerbations of managed chronic conditions, medication-related issues, and dehydration. Each of these conditions can be effectively diagnosed and treated by appropriately trained paramedic teams operating under physician medical direction (instED).
Community Paramedicine Outcome Data
Published evaluations of community paramedicine programs consistently demonstrate meaningful reductions in ED utilization among enrolled populations. A program operated in Houston reported a 44% reduction (University of Texas Health Science Center) in ED visits among high-utilizer patients enrolled in community paramedicine services. A program in Minnesota documented a 38% reduction in 911 calls from its target population over a two-year period.
Clinical quality metrics from these programs are favorable. Patient safety incident rates are comparable to traditional urgent care settings. Paramedic teams operating under physician protocols demonstrate diagnostic accuracy rates above 90% for conditions within their scope of practice. The treat-and-refer model, where paramedics treat the immediate condition and connect the patient with appropriate follow-up care, produces follow-through rates significantly higher than ED discharge referrals.
Economic Impact
The economic case for expanded paramedicine roles is driven by the cost differential between an in-home or community-based paramedic visit and an ED encounter. The average community paramedicine visit generates costs between $300 and $700, compared to average ED visit costs exceeding $2,200. For health plans and hospital systems bearing financial risk for patient populations, each diverted ED visit represents a net savings even after accounting for the full cost of the community paramedicine program.
Medicare Advantage plans have been among the earliest adopters (Medicare Payment Advisory Commission) of community paramedicine partnerships, recognizing that proactive home-based interventions reduce total cost of care for their highest-risk members. Several state Medicaid programs have also initiated community paramedicine coverage (National Association of State EMS Officials), driven by the dual goals of improving access for underserved populations and reducing emergency system costs.
An Evolving Healthcare Role
The expansion of paramedicine beyond traditional emergency response represents a structural adaptation to systemic healthcare delivery gaps. Paramedics possess the clinical training, mobile infrastructure, and community presence necessary to meet patients where they are and deliver effective care for conditions that do not require emergency department resources. As data continues to validate this expanded role, the integration of paramedic-delivered care into the broader healthcare delivery model will continue to grow, reducing preventable ED utilization while improving access and outcomes for patients.